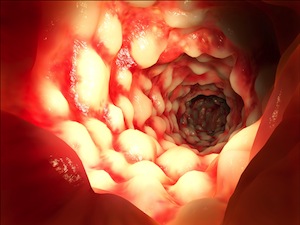
 Crohn’s Disease is chronic irritation of the gastrointestinal tract. It is one of several irritable bowel diseases that share similar symptoms and immune disorders. The lesions that have become an identifying feature of Crohn’s Disease complicate intestinal function. This damage to the gastrointestinal tract can lead to more serious conditions. [1]
Crohn’s Disease is chronic irritation of the gastrointestinal tract. It is one of several irritable bowel diseases that share similar symptoms and immune disorders. The lesions that have become an identifying feature of Crohn’s Disease complicate intestinal function. This damage to the gastrointestinal tract can lead to more serious conditions. [1]
The causes of Crohn’s Disease are under reevaluation. For a while, it was thought that an overactive immune response initiated and the aggravated the condition. Recent studies have suggested the conditions that initiate the disease differ from those that perpetuate it.
Regardless of the cause, Crohn’s Disease requires constant monitoring and attention to ensure the condition does not degrade.
Causes of Crohn’s Disease
 Several theories have developed regarding the cause of Crohn’s Disease. Researchers have explored the involvement of three primary factors: genetic disposition, immune response and gut flora (friendly or unfriendly). As research continues, it appears all three share the development of this chronic bowel disease.
Several theories have developed regarding the cause of Crohn’s Disease. Researchers have explored the involvement of three primary factors: genetic disposition, immune response and gut flora (friendly or unfriendly). As research continues, it appears all three share the development of this chronic bowel disease.
Scientists have identified the NOD2 gene as predisposing an individual to developing Crohn’s Disease. This gene appears to inhibit ‘friendly’ gut flora that help the body maintain a healthy gut, resulting in damage to the lining of the intestines can result. [2]
While an overactive immune response was originally thought to cause Crohn’s Disease, new findings suggest the problem is the exact opposite. A lack of immune response may actually be the cause. [3]Reduced immune response allows harmful bacteria, such as E. Coli to flourish and penetrate into the lining of the intestine leading to irritation, redness, and potentially the commonly observed lesions. [4] [5]
It is worth noting… one other factor has recently been identified with causing complications with Crohn’s Disease: smoking. Smokers suffering from Crohn’s Disease have been found to suffer greater problems than those who don’t, or who quit. Based on the research, any smoker diagnosed with Crohn’s Disease should quit smoking as part of their therapeutic plan. [6]
Symptoms of Crohn’s Disease
The challenge of Irritable Bowel Diseases lies in the recognizing the symptoms reflect a problem with the bowels. Intestinal symptoms of Crohn’s disease include diarrhea, bloating, blood in the stool, and possibly sores in mouth or esophagus, though this is rare. In many situations these symptoms do not occur consistently. Often Crohn’s Disease is recognized only after conditions develop outside the bowel, such as with skin or neurologic disorders.
Dangers of Untreated Crohn’s Disease

In addition, deep vein thrombosis and cancers of the large or small intestine have also been observed. Deep Vein Thrombosis occurs with constant inflammation and is a very serious situation that can result in death. [7] Cancers of the large intestine occur much more frequently than those in the small intestine in patients with Crohn’s Disease. Cancers of the small intestine may be less frequent, but must be watched as Crohn’s Disease may hide indications of the cancer. [8]
What Can Be Done?
To ensure the best outcome, Crohn’s Disease needs to be identified early. Fortunately, individuals who do identify Crohn’s Disease early can live a normal life with expectation of a full lifespan. Improvement typically occurs after a dietary change to prevent consumption of aggravating foods, while ensuring necessary nutrition is consumed. [9]
References (9)
- Baumgart DC, Sandborn WJ. Crohn’s disease. Lancet. 2012 Nov 3;380(9853):1590-605. doi: 10.1016/S0140-6736(12)60026-9. Epub 2012 Aug 20.
- Secher T, Normand S, Chamaillard M. NOD2 prevents emergence of disease-predisposing microbiota. Gut Microbes. 2013 Jun 6;4(4).
- Marks DJ, Rahman FZ, Sewell GW, Segal AW. Crohn’s disease: an immune deficiency state.Clin Rev Allergy Immunol. 2010 Feb;38(1):20-31. doi: 10.1007/s12016-009-8133-2.
- Sasaki M, Sitaraman SV, Babbin BA, Gerner-Smidt P, Ribot EM, Garrett N, Alpern JA, Akyildiz A, Theiss AL, Nusrat A, Klapproth JM. Invasive Escherichia coli are a feature of Crohn’s disease. Lab Invest. 2007 Oct;87(10):1042-54. Epub 2007 Jul 30.
- DJB Marks and AW Segal. Innate immunity in inflammatory bowel disease: a disease hypothesis. J Pathol. 2008 January; 214(2): 260–266. doi: 10.1002/path.2291.
- Lawrance IC, Murray K, Batman B, Gearry RB, Grafton R, Krishnaprasad K, Andrews JM, Prosser R, Bampton PA, Cooke SE, Mahy G, Radford-Smith G, Croft A, Hanigan K. Crohn’s disease and smoking: Is it ever too late to quit? J Crohns Colitis. 2013 Jun 19. pii: S1873-9946(13)00200-6. doi: 10.1016/j.crohns.2013.05.007.
- Kim W, Kang B, Kim BW, Kim JS, Lee HM, Lim EJ, Kim JI, Kang BK, Ji JS, Lee BI, Choi H. Crohn’s Disease Initially Accompanied by Deep Vein Thrombosis and Ulnar Neuropathy without Metronidazole Exposure. Gut Liver. 2013 Mar;7(2):252-4. doi: 10.5009/gnl.2013.7.2.252. Epub 2013 Mar 14.
- Higashi D, Futami K, Kojima D, Futatsuki R, Ishibashi Y, Maekawa T, Yano Y, Takatsu N, Hirai F, Matsui T, Iwashita A. Cancer of the small intestine in patients with Crohn’s disease.Anticancer Res. 2013 Jul;33(7):2977-80.
- Valeria D’Argenio, Vincenza Precone, Giorgio Casaburi, Erasmo Miele, Massimo Martinelli, Annamaria Staiano, Francesco Salvatore, and Lucia Sacchetti. An Altered Gut Microbiome Profile in a Child Affected by Crohn’s Disease Normalized After Nutritional Therapy. Am J Gastroenterol. 2013 May; 108(5): 851–852. Published online 2013 May 6. doi: 10.1038/ajg.2013.46.



11 thoughts on “What is Crohn’s Disease?”